
Overall, there were 3.8% (130/3385) first-eye cataract patients whose preoperative BCVA≥20/40 during the study period. 
Ltd., Osaka, Japan) four times per day for 1 month. Ltd., Osaka, Japan) four times per day for 2 weeks, and pranoprofen (Senju Pharmaceutical Co. Starting 1day after surgery, the patients administered prednisolone acetate (Allergen Pharmaceutical Ireland, Westport, County Mayo, Ireland) and levofloxacin eye drops (Santen Pharmaceutical Co. Cataract surgery was uneventful in all 130 patients. After removing the viscoelastics, the corneal incisions were hydrated. Then, hydrodissection, chopping, and phacoemulsification were performed, followed by irrigation and aspiration of the cortex, and insertion of an aspheric IOL (ZCB00, Abbott Medical Optics, Santa Ana, CA, USA) into the capsular bag. A 2.6 mm clear corneal incision was created after topical anesthesia with oxybuprocaine hydrochloride eye drops (Santen Pharmaceutical Co., Osaka, Japan), and was followed by continuous curvilinear capsulorhexis with a diameter of about 5.5 mm. The KR-1W analyzer could not perform wavefront analysis in posterior subcapsular cataract (PSC) patients because of central opacity.Īll the surgeries were carried out by one surgeon (Prof. The aberrometer also yielded Strehl ratio values from the point spread function (PSF) and modulation transfer function (MTF) curves as indices of the eye's optical quality. The following aberrations were recorded: coma trefoil spherical aberration tetrafoil secondary astigmatism and 3rd order, 4th order, and total HOAs of Zernike polynomials, which were calculated as root mean square values. 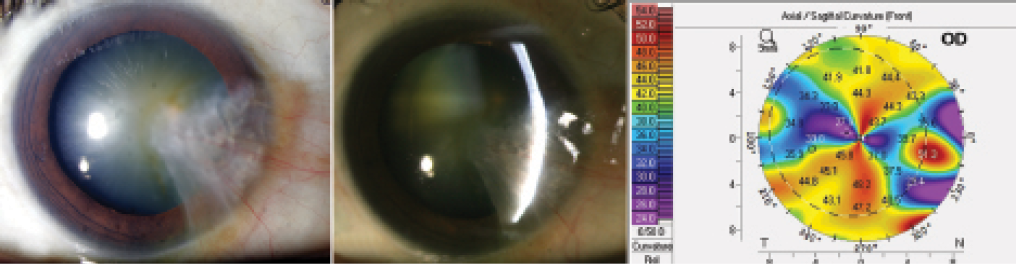
7, 12, 13 Wavefront aberration data were recorded at a pupil diameter of 6 mm. Wavefront aberrometry was performed using a KR-1W analyzer (Topcon, Tokyo, Japan), which simultaneously measures the ocular, corneal, and internal HOAs. After mydriasis, standard anterior segment photographs were taken (Topcon, Tokyo, Japan), and the type and severity of lens opacification were assessed using the Lens Opacities Classification System, version III (LOCS III) by one experienced ophthalmologist (XJZ). Then, the pupils were dilated using Mydrin P (Santen Pharmaceutical Co., Osaka, Japan). UCVA (uncorrected visual acuity), BCVA, and the spherical equivalent (SE) were recorded. Routine ophthalmic examinations, including assessment of visual acuity, refraction, tonometry, fundoscopy, B-scan ultrasonography, and measurement of axial length (AXL) were performed before surgery. With KR-1W, we in the current study evaluated objective functional visual outcomes of cataract surgery in patients with BCVA≥20/40 preoperatively, aiming to determine whether these patients can still benefit from cataract surgery. Although these aberrometers use different measurement principles, they can provide useful information on causes of functional visual complaints in patients with good visual acuity and benefit of cataract surgery. KR-1W, iTrace, and OQASII) can calculate internal aberrations of the eye directly. 6 Previously, cataract surgeons evaluated visual quality mainly through contrast sensitivity and glare disability, which are now thought to be inadequate for these patients, 7, 8, 9, 10 assessment of wavefront data may serve as a good alternative to these conventional tests in patients with good preoperative visual acuity.Īs most internal aberrations of the eye arise from the crystalline lens, aberrometers that can directly measure the internal aberrations allow surgeons to evaluate changes in the internal optical quality of the eye after replacing the cloudy lens with an intraocular lens (IOL). Wavefront analysis has several advantages in providing greater details on high-order aberrations (HOAs) that might cause significant visual disturbances, such as coma and spherical aberration. Therefore, visual acuity seems to provide an inadequate assessment of visual function in these patients. 5 However, there are always a proportion of cataract patients who have good preoperative visual acuity but complain of poor vision. In China, a widely accepted criterion for cataract surgery is that the best-corrected visual acuity (BCVA) of the patient is lower than 20/40. In particular, the Preferred Practice Guideline of the American Academy of Ophthalmology 1 and the RAND Appropriateness Methodology 2 both emphasize the importance of assessing visual function when determining the need for cataract surgery, while other guidelines were based on expert advice. Several groups have developed criteria for cataract surgery. However, the optimal timing of cataract surgery is still unknown. Recent advances in phacoemulsification have greatly improved its risk-to-benefit ratio, allowing surgeons to offer cataract surgery to patients with a low risk of complications.
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
